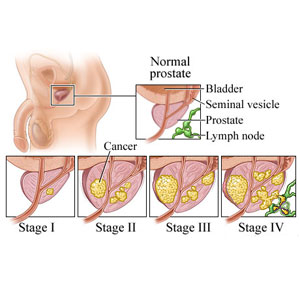
 Everyone knows that testosterone is the main hormone of masculinity, but not everyone knows that it can also stimulate prostate cancer cells growth. So, jabs of testosterone seem something impossible for males suffering this disease.
Everyone knows that testosterone is the main hormone of masculinity, but not everyone knows that it can also stimulate prostate cancer cells growth. So, jabs of testosterone seem something impossible for males suffering this disease.
But the recent research proves that testosterone injections can decrease the growth of these cancer cells in some cases. Since 1940s the studies proved that it has been possible to slow the growth of prostate tumors by decreasing the amount of testosterone and other male sex hormones. Nowadays, a usual way of treating this type of cancer to save other parts of the organism is chemical castration, medicines that stop testosterone and other sex hormones producing. But tumor cells can get used to the testosterone deficit and proceed growing.
For instance, they can crank out of the receptor molecules produced by testosterone or turn to a kind of receptor that can grow without testosterone.
However, the scientists have contrived new ways of treating this opposition, such as medicines that obstruct the receptor of testosterone; cells quickly invent the opposition to them too.
Research of cancer cells during the experiments and in animals has showed a paradox about the prostate cancer of the castration-resistant type. Tumor cells that flourish if the level of testosterone is insufficient die if the hormone level is increased highly. The studies reveal that additional testosterone shatters DNA counterpart and guides to DNA breakage, which is inevitable for a cancer cell. This paradox shows that the dosage of testosterone can bring benefit in fighting cancer-resistant cells.
Michael Schweizer, an oncologist from the University of Washington in Seattle, together with his colleagues at the Johns Hopkins University School of Medicine in Baltimore in Maryland studied this theory with the help of 16 males with prostate cancer-resistant cells. The majority of these cells had expanded or metastasized. During the experiment the males proceed to get chemical castration treatment, but every 28 days the doctors also jabbed them with testosterone. Every jab stimulated the level of testosterone higher than usual, but they decreased to the amount similar to the level typical for chemical castration. The logical explanation for such fluctuation Michael Schweizer saw in the fact that “these prostate cancer cells couldn’t get used to the changing testosterone level.” High testosterone destroys the cells accustomed to a low level, whereas the valleys deter cells that want testosterone to expand.
To test the progress, the scientists gauged the number of prostate-specific antigen (PSA) in blood, which indicates the growth of the cancer. Two of the participants had to leave the experiment after the first stage, as they suffered from some side effects. Seven patients had increased PSA after three stages of the therapy, which showed that they didn’t get any benefit from the shots. But seven of the men had a drooped PSA level, which was a sign that cells might be dwindling. Michael Schweizer comments, “The fact that seven of the fourteen men participated in the study after three stages of the therapy have some progress is promising.”
Schweizer with his colleagues made CT scans on ten males to see whether the size of the metastases generated in comparison with the initial growth. The researchers informed in Science Translational Medicine that four men have a declined amount of metastases, and they disappeared completely in one patient. These five patients were from those with a shrunk PSA level.
Although as time passed, the benefits of testosterone jabs faded. PSA level started to grow in approximately 7 months, which suggested the renewal of cells growing. But even such a short progress can prolong the life of men, as cancer resistant to chemical castration is generally not cured, Michael Schweizer remarks. However, several prior research targeted to measure the effects on cancer of increasing testosterone level, they did not supply the high doses of this hormone to destroy cancer-resistant cells, he admits. So the new study “is the first stage that will help scientists find out who will get an advantage of such a therapy.”
The men who continued the experiment have such side effects as hair loss, nausea, and two of the patients suffered from blood clots in their lungs. One of the two patients who stopped the therapy on the first stage had pneumonia and died in the result of sepsis. Michael Schweizer states that this is not a characteristic consequence of testosterone treatment, so the scientists suppose that his death occurred because of the chemotherapy medicine which the men were taking during the therapy.
Some scientists and oncologists have brooded that testosterone therapy could increase the cancer cells growth, says a cancer endocrinology researcher and physician at the University of California in San Francisco Charles Ryan, who participated in the study. But the research reveals that “there is a good amount of men who benefited from this therapy without any harmful effects.” Although he doesn’t intend to change his methods of prostate cancer treatment till further studies prove the effects of a new therapy and elucidate the possible risks. “The received clinical data are encouraging,” tells Christopher Logothetis from the University of Texas MD Anderson Cancer Center in Houston, who also was among the researchers. But he was saddened that the researchers didn’t make biopsy analysis of the samples to see what impact had testosterone on cancer cells. Biopsy is necessary for the scientists to see how to determine who will get an advantage from the testosterone therapy and who will have negative effects, he explains. Michael Schweizer informs about the start of two more studies of testosterone influence in men with cancer-resistant cells, so this will give the scientists a possibility to understand if testosterone therapy is better than the existed methods of treatment.